What is Inflammatory Bowel Disease (IBD)?

Inflammatory bowel disease (IBD) is a chronic condition characterised by persistent inflammation of the digestive tract. It affects the intestines and can lead to long-term symptoms that fluctuate between active flare-ups and periods of remission.
IBD is a lifelong condition that requires ongoing medical monitoring and personalised treatment to control inflammation, relieve symptoms, and reduce complications.
How Common Is IBD?
While IBD is less common than other gastrointestinal conditions, its prevalence has been steadily increasing globally. Early recognition and specialist care play a key role in managing the disease and improving long-term outcomes.
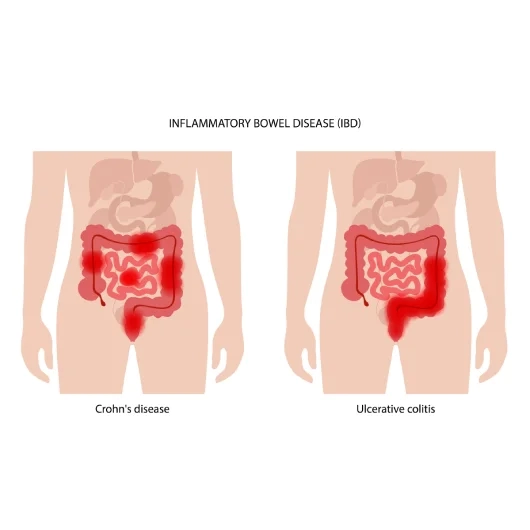
Types of Inflammatory Bowel Disease
There are two main types of IBD:
Crohn’s Disease
Crohn’s disease can affect any part of the digestive tract, from the mouth to the anus, and often involves deeper layers of the bowel wall. Patients may experience variable symptoms depending on disease location.
Ulcerative Colitis
Ulcerative colitis affects the lining of the colon and rectum. Inflammation typically begins in the rectum and may extend upward through the colon. Care for ulcerative colitis focuses on controlling inflammation and preventing flare-ups.
Signs and Symptoms
IBD symptoms may vary depending on the type and severity of the disease. Common symptoms include:
- Persistent diarrhoea
- Abdominal pain or cramping
- Blood or mucus in stool
- Fatigue
- Unintended weight loss
Symptoms may worsen during flare-ups and improve during periods of remission. Early evaluation is crucial to guide appropriate treatment and minimise complications.
Causes and Risk Factors
The exact causes of IBD are not fully understood. It is believed to result from an abnormal immune response, with both genetic and environmental factors contributing to its development.
Common IBD risk factors include:
- Family history of IBD
- Immune system dysfunction
- Environmental triggers
- Smoking (particularly for Crohn’s disease)
Diagnosing Inflammatory Bowel Disease
Diagnosis of IBD involves a combination of clinical evaluation, imaging tests, laboratory work, and endoscopy.
Diagnosis aims to:
- Confirm the presence of inflammation
- Determine the type of IBD
- Assess disease extent and severity
Accurate diagnosis is essential for creating an effective treatment plan and guiding long-term management.
Managing Inflammatory Bowel Disease
IBD management focuses on controlling inflammation, reducing symptoms, and maintaining long-term remission.

Treatment Options
Treatment options vary depending on the type of IBD, its severity, and how the patient responds to treatment. Common approaches include:
- Anti-inflammatory medications: These help reduce inflammation in the gut, managing symptoms like diarrhoea and pain. Examples include aminosalicylates and steroids.
- Immune system-modulating therapy: These medications suppress the overactive immune system to prevent it from attacking the gut. Drugs like azathioprine are commonly used.
- Biologic treatments: Targeted therapies that reduce inflammation by blocking specific molecules in the immune system. Common biologics include TNF inhibitors (e.g., infliximab).
- Nutritional support: Since IBD can affect nutrient absorption, nutritional therapy ensures proper intake of vitamins and minerals, often using special diets or supplements.
There is no cure for IBD, but with the right treatment, many patients can achieve long-term remission.
Possible Complications
Without proper control, IBD complications can arise, including:
- Intestinal strictures (narrowing of the intestines)
- Fistulas (abnormal connections between organs)
- Increased risk of infections
- Nutritional deficiencies
- Higher risk of colorectal cancer over time
Regular follow-up is crucial to detect complications early and adjust treatment plans as needed.
When to See a Doctor
Consult a doctor if you experience:
- Persistent digestive symptoms
- Recurrent diarrhoea or abdominal pain
- Blood in stool
- Unexplained weight loss
Seeing an IBD specialist is important for comprehensive evaluation and tailored treatment, especially if your symptoms are severe, recurring, or not responding to initial treatment.
Book an AppointmentFrequently Asked Questions
No. IBD involves inflammation of the digestive tract, whereas IBS is a functional disorder that does not cause structural inflammation in the bowel.
If not managed properly, IBD can lead to complications such as intestinal strictures, fistulas, malnutrition, and an increased risk of colorectal cancer. Regular monitoring and treatment are essential to reduce these risks.
There is no cure for IBD, but many patients can achieve long-term remission with the right treatment. Managing symptoms and preventing flare-ups are key components of treatment.
In Singapore, IBD treatment is tailored to each patient’s needs. It typically involves medications, lifestyle changes, and, in some cases, surgery. For non-surgical management, patients can see a gastroenterologist who specialises in IBD. If surgery is required, a colorectal surgeon will provide expert care.
People with IBD, particularly long-term ulcerative colitis, may have a higher risk of developing colorectal cancer. Regular screenings and monitoring by your healthcare team can help detect any early signs.










